Nursing While Pregnant: 5 Secrets To Avoiding Agitation And Soreness
For many parents, the journey of breastfeeding is deeply cherished, a profound bond between parent and child. When another pregnancy enters the picture, however, the landscape of nursing can shift dramatically, bringing with it a unique set of physical and emotional challenges. The idea of nursing while pregnant, often referred to as ‘tandem nursing’ if the older child continues to nurse after the new baby arrives, is a topic that sparks curiosity, questions, and sometimes, apprehension. This guide is designed to empower you, whether you are a new parent, a new dad supporting your partner, or a couple trying to conceive, with the knowledge and practical ‘secrets’ to navigate this experience with greater comfort and confidence.
It’s important to acknowledge that experiencing agitation and soreness is incredibly common when nursing during pregnancy. Hormonal fluctuations, changes in milk supply, and increased nipple sensitivity can all contribute to discomfort. You are not alone in these feelings. As a certified Doula and Maternal Health Educator, I’ve supported many families through this unique phase, and I’m here to share five essential strategies that can make a significant difference in your journey. Our goal is not just to manage discomfort, but to foster a sustainable and positive experience for both you and your nursing child, while prioritizing your well-being and the health of your new pregnancy.
Secret 1: Understanding and Adapting to Hormonal Shifts and Nipple Sensitivity

One of the primary drivers of discomfort when nursing during pregnancy is the profound hormonal changes your body undergoes. The surge in progesterone and estrogen, essential for sustaining the pregnancy, can significantly impact your milk supply and, crucially, increase nipple and breast sensitivity. This heightened sensitivity can lead to feelings of agitation, aversion, or even pain during nursing sessions.
Why Hormones Play a Role:
- Progesterone and Estrogen Increase: These hormones prepare your body for the new pregnancy, but they also begin the process of colostrum production, which can alter the taste and amount of your current milk supply.
- Decreased Milk Supply: Many nursing parents notice a drop in milk supply, particularly in the second trimester. This is a normal physiological change and is not a reflection of your body’s ability to produce milk for the new baby.
- Nipple Tenderness: The same hormones that cause morning sickness and breast tenderness in early pregnancy can make nursing feel intensely uncomfortable.
Strategies for Adaptation:
- Gentle Touch and Latch: Encourage your child to latch as gently as possible. If your child is older, you might explain that mommy’s breasts are ‘a little bit sore’ and ask them to be gentle.
- Shorten Nursing Sessions: Consider setting limits on nursing duration. A quick ‘snack’ rather than a long feed might be more tolerable. You can use timers or count to a certain number.
- Distraction Techniques: Engage your child with a story or song during nursing to help them focus and potentially shorten the session without a struggle.
- Wear Loose Clothing: Tight clothing can exacerbate nipple sensitivity. Opt for soft, breathable fabrics.
Secret 2: Effective Communication and Setting Boundaries with Your Child

For your nursing child, the changes in milk taste, supply, and your physical availability can be confusing. Open and age-appropriate communication is vital, as is setting clear, loving boundaries. This approach not only helps manage your discomfort but also prepares your child for the upcoming family changes.
Communicating with Your Child:
- Simple Explanations: For toddlers, use simple language. For example, ‘Mommy’s tummy has a baby, and sometimes my boobies feel a little ouchy when you nurse. We can have short cuddles.’
- Validate Their Feelings: Acknowledge any frustration or sadness they might express about changes in nursing. ‘I know you love nursing, and it’s okay to feel sad that it’s different now.’
- Offer Alternatives: Provide other forms of comfort and connection, such as extra cuddles, story time, special play, or a warm drink.
Setting Loving Boundaries:
- Designate Nursing Times: Establish specific times for nursing (e.g., ‘only at nap time and bedtime’). This helps create predictability for your child and limits your exposure to discomfort.
- Create a ‘Nursing Spot’: Have a designated comfortable chair or area where nursing happens. This can help mentally prepare both of you for the session.
- Involve Your Partner: Your partner can play a crucial role in distraction and comfort during non-nursing times, offering cuddles or snacks when your child seeks the breast. This reinforces that comfort comes from multiple sources.
- Gentle Weaning (If Desired): If the discomfort is too great, or if you feel it’s time, you might consider gentle weaning. This should be a gradual process, often starting with dropping the least desired feed.
Secret 3: Mastering Comfort: Positions, Latch, and Shortened Sessions
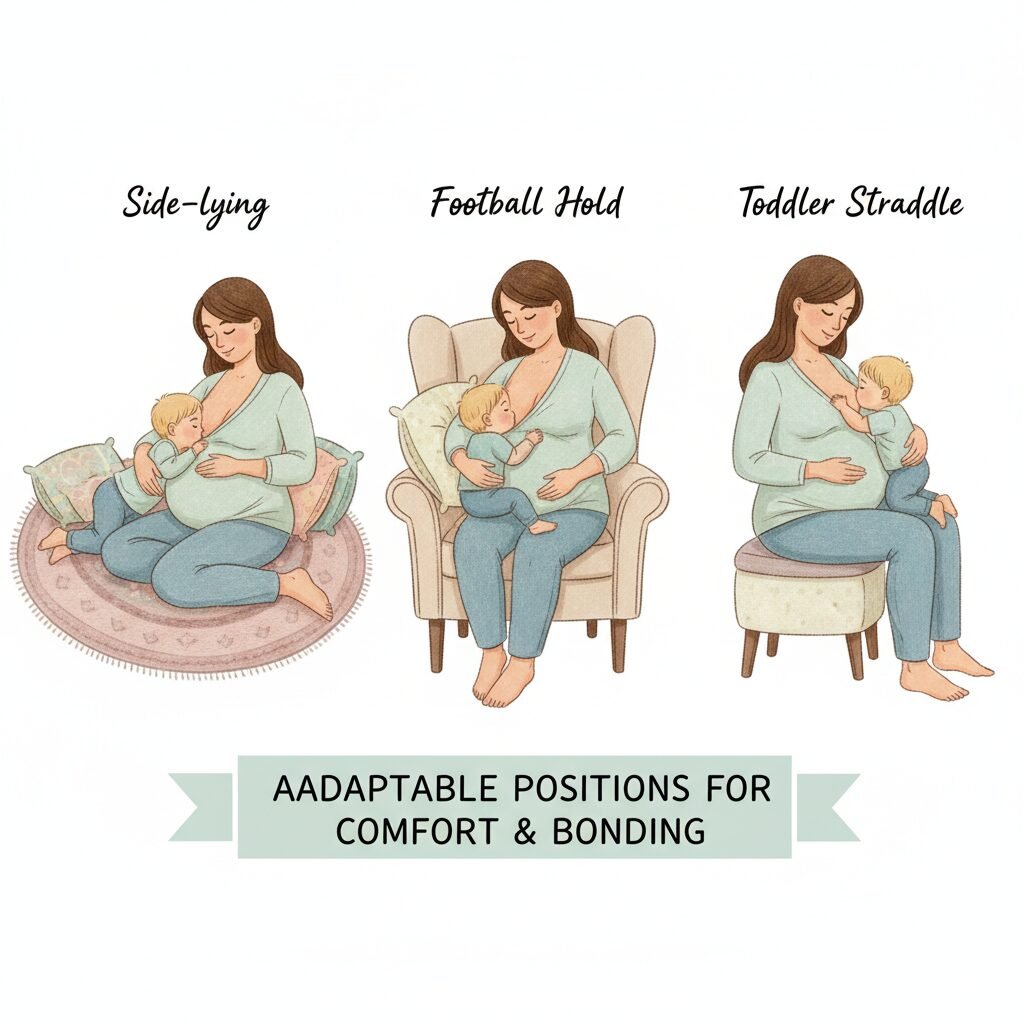
Physical comfort is paramount when nursing while pregnant. As your belly grows, familiar nursing positions may become awkward or even painful. Adapting your technique can significantly reduce both physical soreness and feelings of agitation.
Optimizing Nursing Comfort:
- Experiment with Positions: Find positions that take pressure off your growing abdomen.
| Traditional Position | Pregnancy Adaptation |
|---|---|
| Cradle Hold | Football Hold: Allows your baby to be at your side, keeping pressure off your belly. |
| Cross-Cradle Hold | Side-Lying: Offers maximum rest for you and can be very comfortable. |
| Laid-Back Nursing | Reclining: Semi-reclined position with pillows supporting your back and head can be comfortable. |
| Upright/Straddle Position | Toddler Straddle: Your child sits facing you, straddling your leg or lap, which can minimize direct contact with your belly. |
- Ensure a Deep Latch: A shallow latch can lead to nipple soreness regardless of pregnancy. Re-evaluate your child’s latch to ensure it’s deep and comfortable.
- Pillow Power: Utilize pillows to support your back, arms, and belly. A nursing pillow can still be helpful, even with an older child.
- Shorten Sessions Strategically: As mentioned, shorter sessions can be key. If your child is older, you might explain, ‘We’ll nurse for three songs,’ or ‘just until mommy counts to twenty.’
- Use Distraction: Keep a book or toy handy to gently distract your child if they tend to linger at the breast beyond what is comfortable for you.
Secret 4: Prioritizing Your Well-being: Nutrition, Hydration, and Rest

Nursing during pregnancy places additional demands on your body. It’s not just about nourishing your developing baby, but also continuing to support your nursing child and yourself. Neglecting your own needs can exacerbate feelings of fatigue, agitation, and overall discomfort.
Holistic Self-Care Strategies:
- Boost Your Nutrition: You are essentially nourishing three bodies – yourself, your nursing child, and your developing baby. Ensure you are consuming enough calories (an additional 500-650 calories per day if nursing and pregnant) and nutrient-dense foods. Focus on whole grains, lean proteins, fruits, and vegetables.
- Stay Exceptionally Hydrated: Water is crucial for milk production and overall bodily function. Keep a water bottle with you at all times and sip throughout the day. Dehydration can worsen fatigue and headaches.
- Prioritize Rest: While easier said than done with a little one, finding moments for rest is vital. Nap when your child naps, accept help with household chores, and delegate tasks to your partner or support system. Even 15-20 minutes of quiet rest can make a difference.
- Gentle Pain Management: For nipple soreness, consider using a warm compress before nursing or applying a soothing lanolin cream or breast balm after. Consult with your healthcare provider or a lactation consultant for safe pain relief options during pregnancy.
- Mindfulness and Relaxation: Practices like deep breathing, gentle stretching, or short meditations can help manage the emotional agitation that sometimes accompanies physical discomfort.
“Your body is doing incredible work growing a new life while nourishing another. Extending compassion and prioritizing your own well-being isn’t selfish; it’s essential for your health and the health of your family.” – Certified Doula Perspective
Secret 5: Building Your Support System and Knowing When to Seek Help

You don’t have to navigate nursing while pregnant alone. A strong support system, both personal and professional, can provide invaluable assistance, validation, and practical solutions. Knowing when and where to seek help is a critical ‘secret’ to a more positive experience.
Leveraging Your Support System:
- Involve Your Partner: Share your feelings and discomforts openly with your partner. Discuss ways they can support you, whether it’s taking over bedtime routines, providing distractions for your child, or simply offering a listening ear and a shoulder massage.
- Connect with Other Parents: Seek out local or online support groups for tandem nursing or nursing during pregnancy. Hearing from others who understand your experience can be incredibly validating and provide new ideas.
- Lean on Friends and Family: Don’t hesitate to ask for help with meals, childcare, or errands. Even small acts of support can significantly reduce your burden.
When to Seek Professional Guidance:
- Lactation Consultant: If you’re experiencing significant pain, concerns about your child’s nutrition due to decreased milk supply, or simply need tailored advice on positions and strategies, a certified lactation consultant (IBCLC) is your best resource.
- Obstetrician/Midwife: Always inform your healthcare provider that you are nursing while pregnant. They can monitor your pregnancy, ensure adequate nutrition, and address any concerns regarding uterine contractions or other pregnancy-related issues. While nursing generally does not cause preterm labor in a healthy, low-risk pregnancy, it’s essential to keep your provider informed.
- Mental Health Professional: If feelings of agitation, aversion, or emotional distress become overwhelming, persist, or impact your daily life, please reach out to a therapist or counselor specializing in maternal mental health. Your emotional well-being is just as important as your physical health.
Conclusion
Nursing while pregnant is a testament to the incredible strength and adaptability of the human body and spirit. While it can undoubtedly bring moments of agitation and soreness, remember that these feelings are normal, valid, and manageable. By understanding the physiological changes, communicating openly with your child, prioritizing comfort, nurturing your own well-being, and building a robust support system, you can transform this unique phase into a more peaceful and fulfilling experience.
Every journey is unique, and there is no single ‘right’ way to do this. Be kind to yourself, listen to your body, and celebrate the beautiful connections you are fostering. You are doing amazing work, and with these five secrets, you are better equipped to navigate this special time with confidence and grace. For any persistent concerns about your health or your baby’s development, always consult with your healthcare provider.
Disclaimer: This article provides general information and recommendations and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician, midwife, or other qualified health provider with any questions you may have regarding a medical condition or before starting any new treatment or health regimen. The information provided herein is for educational purposes only.







