Master the Latch: Everything You Need to Know Before the First Feed
Welcome, expectant parents. As you prepare to meet your little one, your mind is likely filled with a mix of excitement and a long list of questions. Among the most common concerns is feeding your baby. For those who choose to breastfeed, one word often surfaces with a sense of anxiety: the latch. You may have heard that it’s the key to everything, and in many ways, that’s true. A proper latch is the foundation of a comfortable, effective, and sustainable breastfeeding relationship. It ensures your baby gets the nourishment they need to thrive and protects you from pain and complications.
But here is a truth we must start with: breastfeeding is a learned skill for both you and your baby. It’s a dance you learn together. This guide is designed to be your prenatal class, your trusted resource, and your reassuring voice in the quiet moments before your journey begins. We will demystify the latch, breaking it down into understandable concepts and actionable steps you can learn before your baby is in your arms. Our goal is to replace apprehension with knowledge and confidence, empowering you to navigate the first feed and beyond with grace.
Understanding the ‘Why’: The Critical Importance of a Good Latch
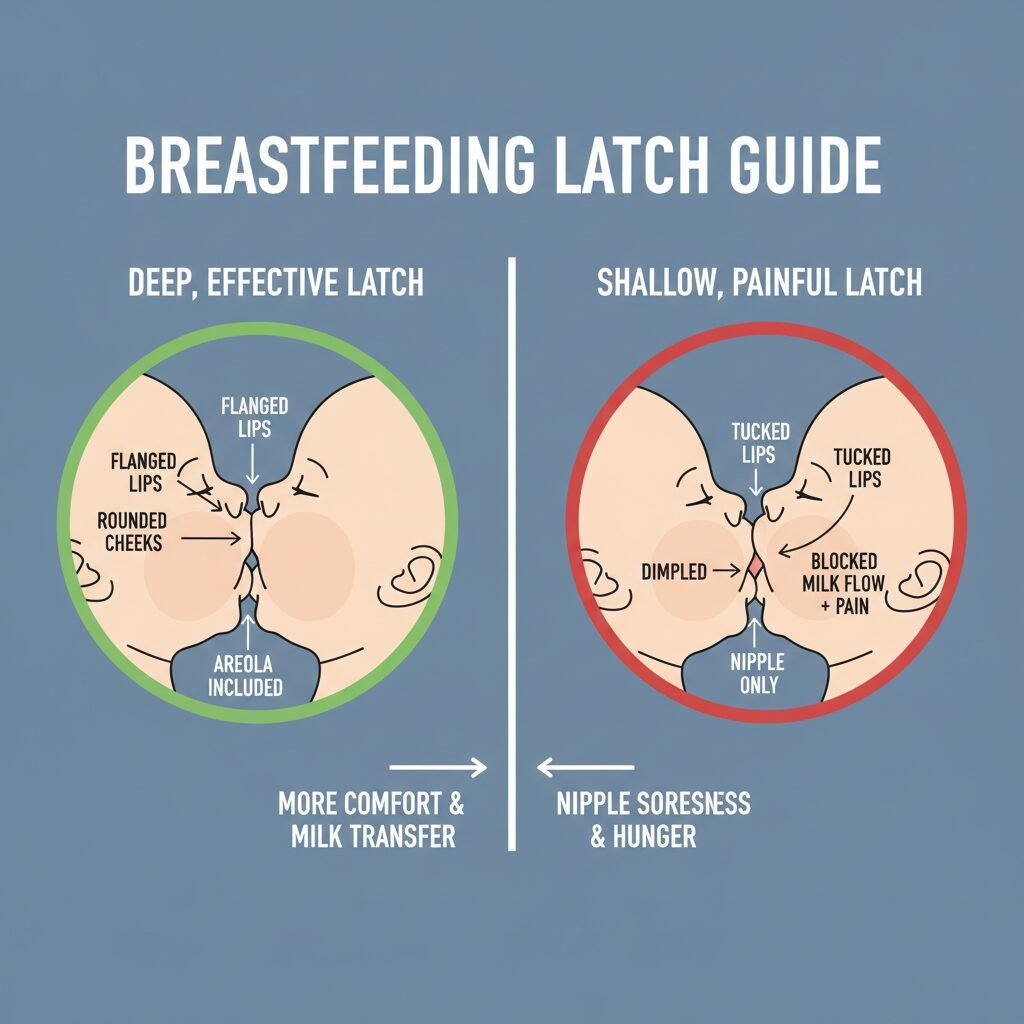
Before we dive into the ‘how,’ it’s essential to understand the ‘why.’ Why is so much emphasis placed on this single aspect of breastfeeding? A successful latch is far more than just getting the baby to attach to the breast; it’s a complex physiological interaction that triggers a cascade of benefits for both parent and child.
Milk Transfer and Infant Nutrition
The primary goal of feeding is, of course, nourishment. An effective latch allows your baby to use their tongue and jaw to draw milk from the breast efficiently. When a baby has a deep latch, their tongue massages the milk ducts located deep within the breast tissue, stimulating the ‘let-down’ reflex and facilitating a steady flow of milk. A shallow latch, in contrast, means the baby is only sucking on the nipple, which is an inefficient and often frustrating way to feed, leading to poor weight gain and a hungry, fussy baby.
Establishing and Maintaining Milk Supply
Breastfeeding operates on a powerful principle of supply and demand. The more milk that is effectively removed from the breast, the more milk your body is signaled to produce. A good latch ensures the breasts are emptied thoroughly, sending a strong message to your brain to keep production high. Conversely, a poor latch that prevents complete milk removal can signal to your body that less milk is needed, potentially leading to a dwindling supply over time.
Parental Comfort and Nipple Health
Let’s be unequivocally clear: breastfeeding should not be painful. While some initial tenderness in the first few days is common as your body adjusts, persistent, sharp, or excruciating pain is a red flag for a poor latch. When a baby latches onto the nipple instead of the areola, the delicate nipple tissue can become compressed, leading to cracks, blisters, and bleeding. This pain can make breastfeeding an ordeal and is a primary reason many parents stop sooner than they intended. A deep, comfortable latch is the number one preventative measure against nipple trauma.
“Think of the latch as the key that unlocks the entire breastfeeding relationship. Without the right key, the door remains stuck. With it, a world of connection and nourishment can open up effortlessly.” – Certified Lactation Consultant
Anatomy of a Perfect Latch: Key Signs to Look and Listen For

Knowing what a good latch looks and feels like is the first step to achieving one. When you bring your baby to the breast, you’ll become a detective, looking for specific cues. We can break these down into a simple checklist. A comfortable, effective latch will typically display most, if not all, of these signs.
Visual Cues: What to See
- A Very Wide Mouth: The baby’s mouth should be open as wide as if they are yawning, not pursed like they’re sipping through a straw. Their gape should be around 140 degrees.
- Flanged Lips: Both the top and bottom lips should be turned outward, like a fish. You may need to gently flip the top or bottom lip out if it’s tucked in.
- Asymmetrical Areola Coverage: You should see more of your areola (the darker skin around the nipple) above your baby’s top lip than below their bottom lip. This indicates the baby has a large mouthful of breast tissue.
- Chin and Nose Position: The baby’s chin should be pressed firmly into the breast, while their nose is just touching or slightly away from it. This ‘sniffing’ position helps them breathe easily.
- Rounded Cheeks: Your baby’s cheeks will be full and rounded, not dimpled or hollowed out, as they suckle.
Auditory and Sensory Cues: What to Hear and Feel
- Rhythmic Sucking Pattern: You’ll notice a pattern of quick sucks to trigger your let-down, followed by long, deep, rhythmic sucks with pauses for swallowing.
- Audible Swallowing: You should be able to hear soft ‘kah’ sounds as your baby swallows milk. Clicking, smacking, or popping sounds often indicate the baby is losing suction and has a shallow latch.
- Absence of Pain: This is the most important cue for you. After the initial pull of the latch-on, feeding should be comfortable. It should feel like a tug or pull, not a pinch or a sharp pain.
| Sign of a Good Latch | Sign of a Potential Problem (Shallow Latch) |
|---|---|
| Mouth is open very wide | Mouth is barely open, lips are pursed |
| Lips are flanged outward | Lips are tucked or rolled inward |
| Feels like a strong tug or pull | Feels like a pinch; sharp, shooting pain |
| Audible swallowing sounds | Clicking or smacking sounds |
| Baby’s cheeks are full and rounded | Baby’s cheeks are dimpled or hollow |
| Baby is content and settled after feeding | Baby is fussy, seems hungry after feeding |
Your Pre-Baby Latch Practice Plan: Preparing Body and Mind

You don’t have to wait until your baby arrives to start preparing for breastfeeding. Just as you prepare a nursery, you can prepare your mind and support system for a successful start. Taking proactive steps can make a significant difference in your confidence and ability to troubleshoot in the early days.
- Get Educated: Knowledge is power. Attend a prenatal breastfeeding class, either in person or online. These classes, often taught by lactation consultants (IBCLCs), provide evidence-based information and allow you to ask questions. Watch videos from trusted sources that show real mothers and babies latching.
- Learn About Your Anatomy: Familiarize yourself with your own breasts. Do you have flat or inverted nipples? Knowing this beforehand allows you to learn techniques or have tools (like a nipple shield, used under guidance) ready if needed. A lactation consultant can assess this during pregnancy.
- Practice Hand Expression: In the last few weeks of pregnancy (with your provider’s approval), you can learn to hand-express colostrum. This incredible ‘liquid gold’ can be collected and saved for your baby. More importantly, this practice helps you become comfortable handling your breasts and understand where your milk comes from.
- Assemble Your Support Team: Breastfeeding is not a solo act. Your most important team member is your partner. Discuss your breastfeeding goals with them. Educate them on what a good latch looks like so they can be your second set of eyes. Identify a lactation consultant or a local support group (like La Leche League) you can call for help. Have their number ready.
- Create a ‘Nursing Nook’: Designate a comfortable space in your home for feeding. Equip it with a supportive chair, pillows (including a dedicated nursing pillow), a side table for a large water bottle, healthy snacks, your phone, and a burp cloth. Having everything within arm’s reach reduces stress and allows you to focus on your baby.
The First Feed: A Step-by-Step Guide to Latching in the Golden Hour

The ‘golden hour’—the first hour or two after birth—is a magical time. Your baby is often in a quiet, alert state, and their instincts to root and suck are incredibly strong. This is an ideal time for the first feed. Here’s a step-by-step guide to navigating it, whether it’s in the first hour or the tenth.
- Get Comfortable (Positioning is Everything): Before you even pick up your baby, get yourself into a comfortable, well-supported position. Use pillows to support your back, arms, and lap. A laid-back, semi-reclined position is often easiest at first, as it uses gravity to help the baby stay on the breast.
- Position Your Baby (Tummy-to-Mummy): Hold your baby close, with their entire body facing yours. Their chest should be against your chest. Their head, neck, and back should be in a straight line—not with their head turned to the side. Support their neck and shoulders, not the back of their head, to allow them the freedom to tilt their head back.
- Align Nose to Nipple: Bring your baby up to the breast, aligning their nose directly across from your nipple. This encourages them to tilt their head back and reach up for the breast, which naturally helps them get a deeper latch with their bottom jaw.
- Encourage a Wide Gape: Gently tickle your baby’s top lip with your nipple. This will trigger their rooting reflex. Be patient and wait for them to open their mouth very wide, like a big yawn. Avoid trying to latch them when their mouth is only partially open.
- Bring Baby to Breast, Not Breast to Baby: Once their mouth is wide open, use the hand supporting their shoulders to bring them swiftly and assertively onto the breast. The motion should be quick and decisive. Aim to get as much of the lower areola into their mouth as possible.
- Assess and Adjust: Once latched, do a quick mental check. Does it hurt? Are their lips flanged? Is their chin pressed into your breast? If it’s painful or clearly shallow, don’t suffer through it.
- How to Unlatch Correctly: To unlatch, never just pull the baby off, as this can cause nipple damage. Instead, gently slide your clean pinky finger into the corner of their mouth, between their gums, to break the suction. Then, you can remove them from the breast and try again. It is completely normal to have to re-latch several times to get it right.
The Partner’s Crucial Role: How Dads and Support Persons Can Help

To the dads and partners reading this: you are not a bystander in this process. You are an essential part of the breastfeeding team, and your support can dramatically impact success and duration. While you may not be the one physically feeding, your role is active, not passive.
Become the Latch Coach
You have a different vantage point. You can often see the baby’s mouth and lip position more clearly than the nursing parent. Learn the signs of a good latch from this article. Be a gentle, encouraging second set of eyes. You can say things like, “It looks like his bottom lip is tucked in, let’s try to flip it out,” or “That looks so much deeper than last time!”
Master the Environment
Be the master of the nursing nook. Before your partner even sits down to feed, ask, “Do you have your water? Your phone? Do you need another pillow?” Anticipating these needs prevents the nursing parent from having to unlatch a sleeping baby just to grab a snack. This simple act of service is profoundly helpful.
Provide Physical and Emotional Support
During marathon cluster-feeding sessions, your presence is a lifeline. Offer a shoulder rub. Bring food and drink. Tell your partner what an amazing job they are doing. When they are exhausted and doubting themselves at 3 a.m., your words of encouragement—”We’re a team, and you’re doing great. How can I help?”—can be the fuel that gets them through.
Take Over Other Duties
One of the best ways to support breastfeeding is to take ownership of other baby-related tasks. Become the expert diaper-changer, the master swaddler, the chief baby-wearer, and the go-to for burping. This allows the nursing parent to focus their energy on feeding and recovery, knowing that all the other needs are being met by their capable partner. Your contribution creates the peaceful environment necessary for breastfeeding to flourish.
Conclusion
Mastering the latch is a journey, not a destination. There will be perfect feeds, and there will be fumbling, frustrating attempts—sometimes in the same day. Give yourself and your baby an abundance of grace. Remember that you are both learning a new, intricate dance together. The preparation you do now, by reading articles like this one, is an incredible gift to your future self.
Celebrate the small victories. Trust your instincts. And above all, do not hesitate to ask for help. A lactation consultant is a priceless resource who can provide personalized, hands-on support to solve any challenges you encounter. You are building a foundation of nourishment and connection that will last a lifetime. You can do this.
Medical Disclaimer: The information provided in this article is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician, pediatrician, or other qualified health provider, such as an International Board Certified Lactation Consultant (IBCLC), with any questions you may have regarding a medical condition or breastfeeding.







